In a North Carolina ICU, hopes are muted as COVID continues to prey on the vulnerable
There are encouraging signs about the latest wave of COVID-19. New cases in South Africa, where the omicron variant of the coronavirus was first identified, have fallen steeply since late December, and the same is starting to happen in parts of the United States.
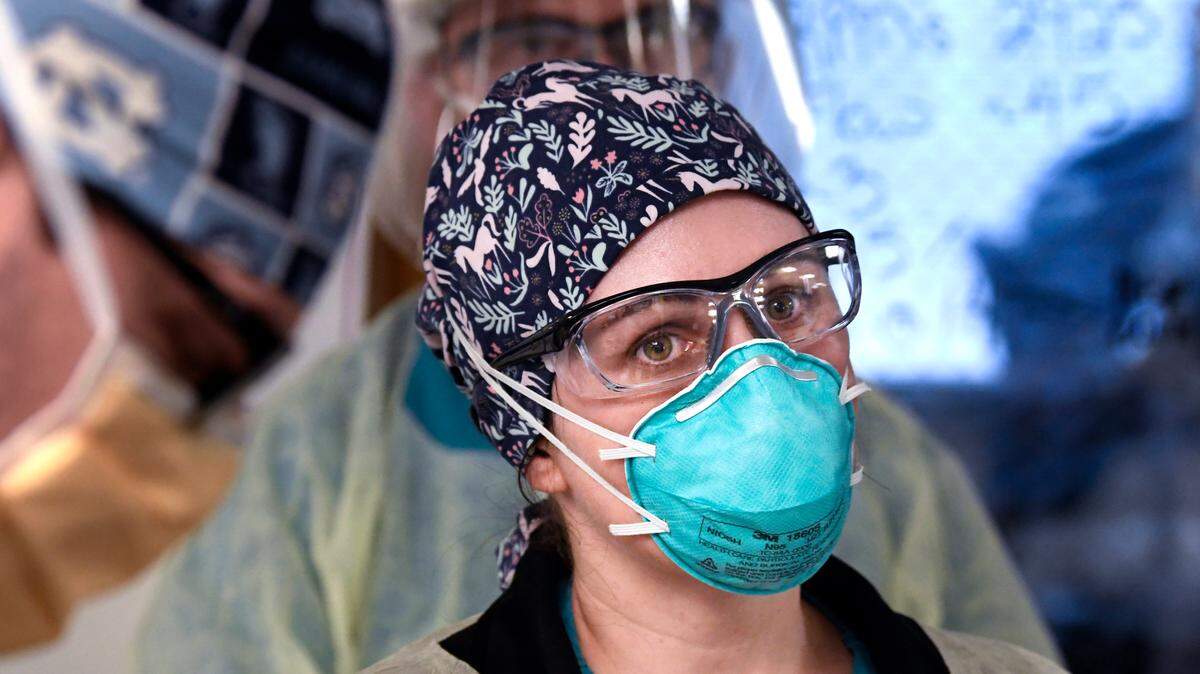
But Katie Creran isn’t confident that an end to the pandemic is in sight. Creran is a registered nurse in the surgical/trauma intensive care unit at UNC Medical Center, where the most seriously ill COVID-19 patients are treated.
Here, the patients receive what’s known as ECMO or extracorporeal membrane oxygenation. They’re heavily sedated and hooked up to ECMO machines that provide oxygen directly to their blood because the virus has so damaged their lungs that even mechanical ventilation isn’t enough.
Patients on ECMO require round-the-clock attention from people like Creran, who has worked in this ICU for six years. Like many who care for COVID-19 patients, she thought the arrival of vaccines last year meant an end to the pandemic was coming.
Then came a backlash to the vaccines, and vaccination rates stalled. Fewer than half of adults 18 and older in North Carolina are fully vaccinated and boosted against the coronavirus, according to the state Department of Health and Human Services. Creran says she’s “kind of given up hoping” the pandemic will end.
“Things might get better for a little while, and then a new variant comes out and we still don’t have the herd immunity we need to be able to keep people out of the ICU,” she said Thursday, standing outside the room of a COVID patient receiving ECMO. “I just guard my hope pretty close to the chest.”
Where to find ECMO treatment in NC?
ECMO is only available at large medical centers; in the Triangle, Duke and WakeMed also offer the treatment for COVID-19.
UNC has one of the nation’s largest programs, said Dr. Lauren Raff, a surgeon and trauma doctor on the team that treats patients with ECMO. Before COVID-19, UNC used the procedure with heart and lung patients about two dozen times a year, Raff said.
About 160 COVID-19 patients have required ECMO at UNC since the pandemic began in the spring of 2020. At the peak of last summer’s surge of the delta variant, 13 of the 16 beds in the surgical/trauma ICU were filled with patients on ECMO.
On Thursday, four patients in the ICU were receiving ECMO for COVID-19. Like those who came before, they had underlying health problems, such as hypertension or diabetes, that made them vulnerable to the virus, and none of them had been vaccinated against the virus, Raff said.
Though there are exceptions, it’s rare that a vaccinated patient will get sick enough to need a ventilator, let alone ECMO.
“Everything has shown, since the advent of the vaccine, that generally it is very safe and is exceedingly effective at preventing severe illness from COVID,” Raff said.
The omicron variant has fueled a spike in hospitalizations for COVID-19, hitting a record 5,158 patients statewide on Thursday, according to DHHS. But in general the variant causes less severe illness; fewer than 16% of those patients were in hospital ICUs, compared to nearly a third during the delta surge last summer.
The UNC Medical Center had 160 COVID-19 patients Thursday, including 25 who needed intensive care.
Raff knows of only two UNC patients infected with the omicron variant who have needed ECMO; the rest in her ICU were hit by the delta variant, which is still circulating, she said. Doctors hope the prevalence of omicron will reduce the number of severely ill patients even further, Raff said.
“But the fear that we have is what is coming after omicron,” she said. “So long as there’s a large unvaccinated population, this virus can mutate and can change very quickly and can spread very quickly. It’s proven that over and over again.”
Most COVID patients on ECMO won’t survive
For COVID patients, ECMO is a treatment of last resort. A patient can remain on the machine for anywhere from 10 days to seven weeks while their body tries to heal the damage to their lungs, Raff said. About 60% of ECMO patients won’t survive.
Creran said people who work in the ICU normally get to see “a decent amount of happy endings” as patients recover from surgery or trauma and go home. It’s hard watching so many die of COVID-19, she said.
“We have to build up a certain wall against these emotions,” she said. “We all have to come up with our own way coping to deal with it and try to distance ourselves from it, unfortunately. Just for our own self preservation.”
When COVID-19 patients arrive in the ICU, they’re already heavily sedated and on ventilators. If ECMO is successful, the patients are still sedated when they leave.
That means Creran and her coworkers never see their COVID-19 patients when they’re conscious. What they know about them comes only from medical charts and what visiting family members tell them.
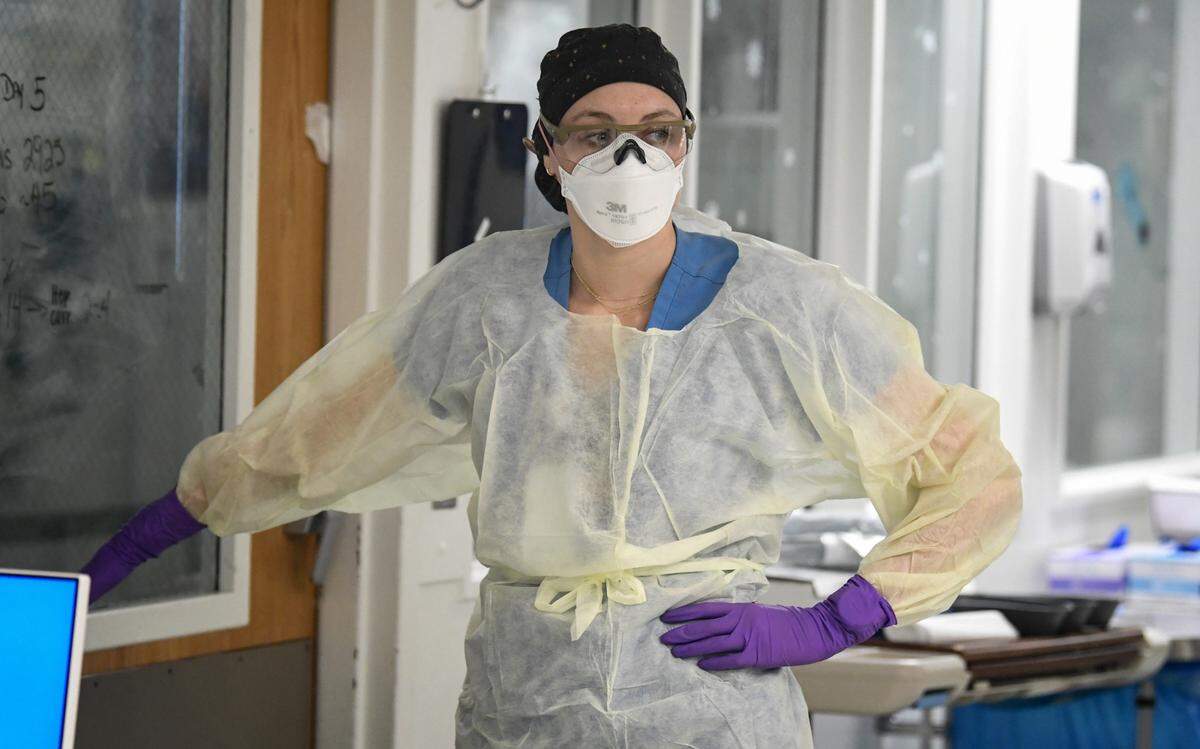
Creran works three 12-hour shifts a week, often caring for the same patient each time. She monitors her patient and the ECMO machine almost constantly; makes sure that food and liquids are going in and urine and feces are coming out, all through tubes; moves the patient every two hours to prevent skin damage; and gives them a sponge bath once a day.
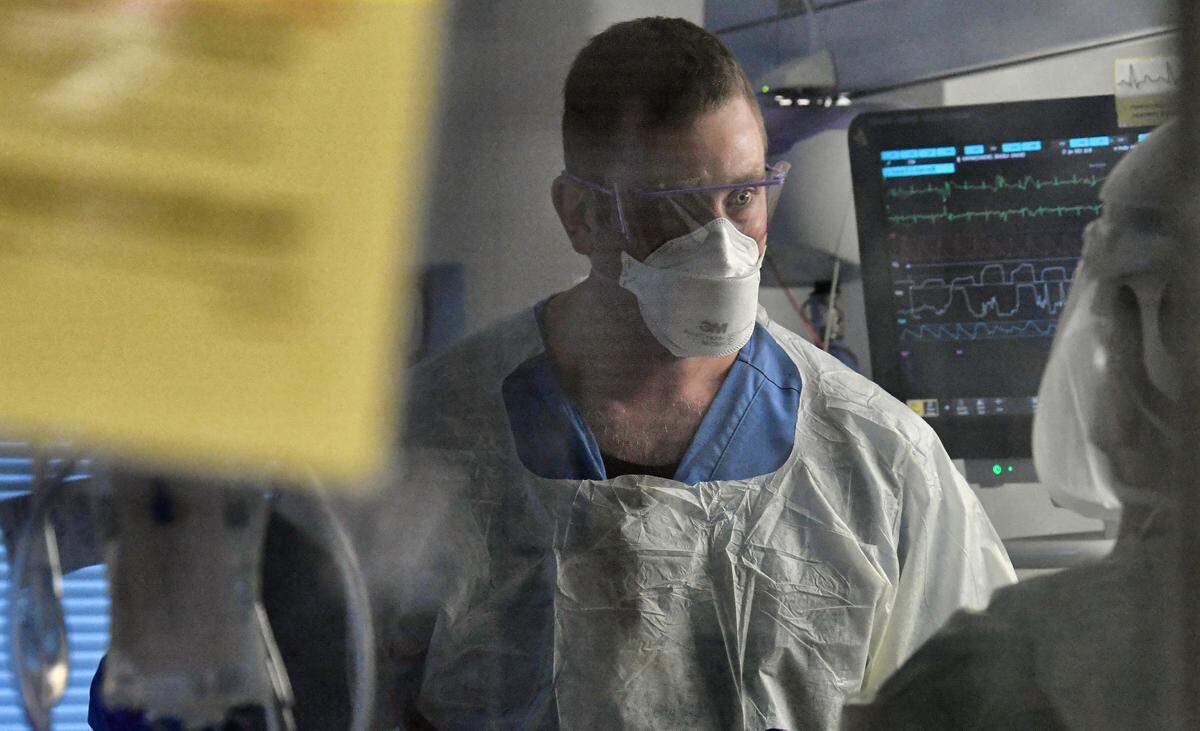
On Thursday morning, Raff, Creran and a half dozen others involved with her patient huddled outside his room to go over his progress and update their strategy. Raff suggested they adjust his sedation and consider another “trial,” where the amount of blood flowing through the ECMO machine is scaled back to see if he’s able to get enough oxygen from the ventilator alone.
A previous trial two days earlier showed that he wasn’t ready.
Ongoing coronavirus fight is ‘frustrating’
Like many health care workers who treat COVID-19 patients, Creran and Raff are disheartened that so many people distrust the science behind the vaccines and refuse to get vaccinated.
“It’s frustrating to walk around in the world and be on social media and see that people are not believing in it or are still hesitant,” Creran said.
Raff said not knowing when the pandemic will end has worn on doctors, nurses and other health care providers. It has to end sometime, she said.
“We hope it’s over soon,” she said. “We’ll obviously keep going if it’s not.”
This story was originally published January 28, 2022 at 8:40 AM.
