Duke University doctors perform first-of-its-kind heart transplant
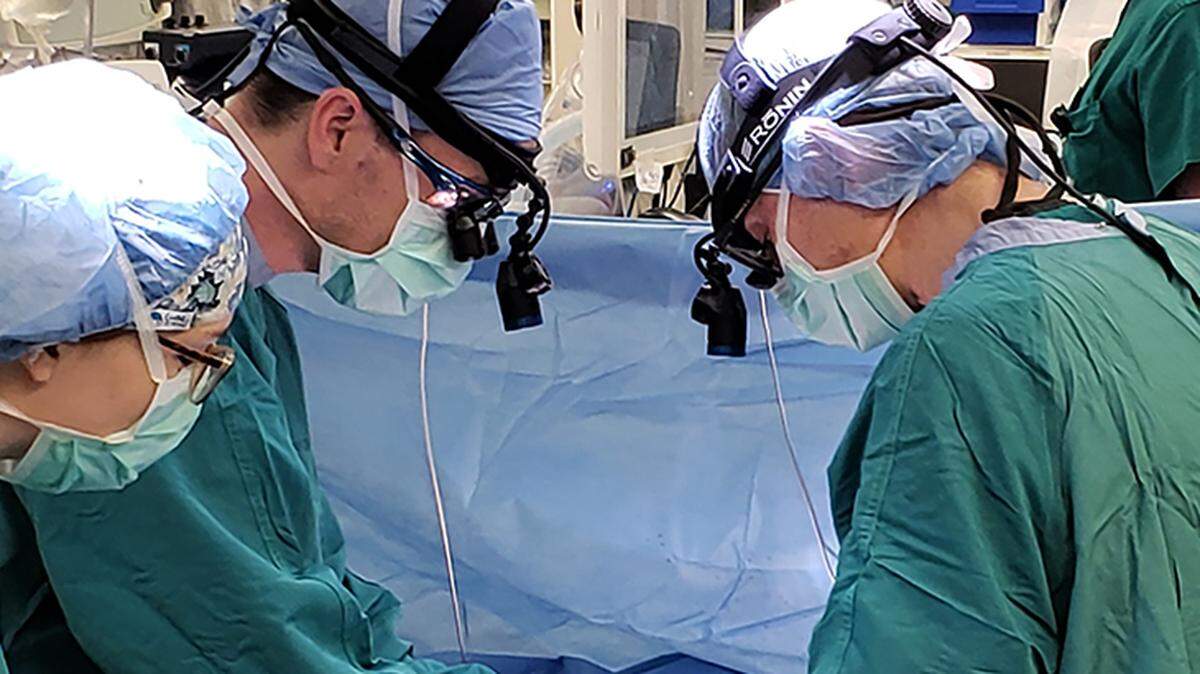
A team of doctors at Duke University became the first in the U.S. to perform a new type of heart transplant surgery this week, launching a study into a new approach to heart donations that could significantly expand the donor pool for transplants.
In the U.S., heart donations have traditionally come after a donor has been medically declared brain dead but still has blood circulation due to life support machines. That was necessary because of how quickly organs deteriorate once circulation stops.
But in a new approach, Duke doctors were able to do a transplant after a donor’s heart stopped beating. The process is called donation after circulatory death, or DCD, and is only being done in the U.S. now because of a recently launched clinical trial of a device that can reanimate organs after circulation has stopped.
The device, TransMedics Group’s Organ Care System, resuscitates the heart mere minutes after it has stopped beating by circulating warm, oxygenated blood through it, helping prevent damage.
DCD donations have been performed previously in the U.K. and Australia, but the device needed to perform the surgery hasn’t yet gotten widespread approval from the U.S. Food and Drug Administration, said Dr. Jacob Schroder, an assistant professor of surgery at Duke University who performed the surgery.
Schroder noted in the past there had been a pair of pediatric DCD donations in the U.S., and the process has been used to transplant other organs, like kidneys. But the heart is much more susceptible to damage from a loss of circulation than other parts of the body. In these cases, a few minutes can matter for how strong a heart might be after transplant.
He said the new study is significant because it could expand the donor pool by 30% — potentially helping thousands of people waiting on the donor list.
“In this country, at this point, there’s probably about 250,000 people who technically could qualify for a heart transplant,” Schroder said. “Many of them, maybe, are too old or have other problems and wouldn’t necessarily qualify, but technically that’s how many people who could.”
Yet, while the demand for heart transplants is high, only around 3,000 heart transplants are done per year, he noted.
“So, there’s a huge disparity between the number of people who need a transplant and those who get one,” he said. “The reason for that is a lack of suitable donors, and so doing things like ... donation after circulatory death is going to have a major impact.”
A different procedure
Dr. Evan Pivalizza, chair of the American Society of Anesthesiologist’s Committee on Transplant Anesthesia, said that while DCD transplants are seen as a positive step in the medical community, he thinks it’s important the public is educated about the nature of the procedure.
“We want to make sure [people] understand this is a normal dying process,” he said. “Instead of it happening in the intensive care unit or wherever else, it is happening in the operating room, but it’s exactly the same process. It’s just we are waiting to see if the patient passes, then we can attempt to harvest the organs.”
While patients eligible to become DCD donors have no chance for recovery, they have not met the threshold for brain death.
“Most of these patients have had some devastating neurologic injury, but don’t meet the strict criteria for brain death,” Schroder said. “So they’re sort of in limbo in that they have devastating medical problems and are being kept alive only by significant life support, such as requiring mechanical ventilation and medications to keep their blood pressure up.”
With no chance for survival it is up to the wishes of the patient or the family to decide that it is the right time for withdrawal of life support — and whether they want to donate the organs.
If they choose to, then doctors prepare for the surgery. However, there can be no interaction between the doctors performing withdrawal of life support and the surgeons who will do the transplant.
The surgeons have to be in a separate room, by rule, and there is a mandatory waiting time — sometimes five minutes after the heart has stopped beating — between a determination of death and when a surgeon can touch the body.
“The people making the determination are not involved in the organ donation process, so there are two independent processes,” Pivalizza said. “You never want anyone to turn around and say, ‘Hey, you made the determination of death and then you harvested the organs.’ That would be a conflict of interest and that would be unethical.”
A very busy few hours
The first adult DCD operation occurred on Sunday, with Schroder and Dr. Benjamin Bryner traveling to the donor’s hospital to perform the operation. They learned about the possibility of the donation approximately 18 hours before it happened. From there everything moved very quickly.
At the donor’s hospital, life support was withdrawn and the donor died around five minutes later. Then came the brief waiting period, where a doctor at that hospital pronounced the death.
Then the act to quickly save the heart started.
“When the patient is pronounced dead, then we very quickly procure the organs which, frankly, doesn’t take that much time,” Schroder said. “It takes about 10 minutes to infuse the heart with a cold solution that sort of preserves it, and then [we] remove the heart.”
For the next hour, the doctors hook the heart up to the TransMedics device to resuscitate it and take measurements to confirm that the heart is suitable for transplant and can safely be transported.
“It is a very busy few hours,” he said.
Back at Duke, Dr. Carmelo Milano prepared the transplant recipient for the new heart, which remained beating inside the TransMedics machine. The new heart was then “put back to sleep,” then implanted in the recipient, which took about an hour. Then doctors began the process of weaning the heart and patient off a machine that had been functioning as heart and lungs.
The recipient, who was described only as a military veteran, is recovering well from the surgery, Duke said in a news release.
It should be the first of many such transplants.
The TransMedics clinical trial aims to collect data on more than 200 patients in the next two years — with Duke as one of five centers in the United States approved to perform the DCD transplants. The procedure will then be evaluated on the survival rates of recipients in five years and how well the hearts function compared to traditional transplant methods.
“I really hope that [DCD] transplants become much more commonplace,” Schroder said.
This story was produced with financial support from a coalition of partners led by Innovate Raleigh as part of an independent journalism fellowship program. The N&O maintains full editorial control of the work. Learn more; go to bit.ly/newsinnovate
This story was originally published December 4, 2019 at 3:20 PM.