Small NC hospital struggles with COVID onslaught. ‘Everywhere is just at max capacity.’
During the first peak of COVID-19 last winter, the emergency department at UNC Health’s hospital in Clayton was busy but not overwhelmed. Many patients with non-COVID problems, such as diabetes or heart disease, were simply avoiding hospitals.
That’s not the case now. People with chronic health conditions began showing up at the emergency room again this spring, many with problems that had grown worse without attention during the coronavirus pandemic.
And then COVID-19 returned, more swiftly and ferociously than it arrived last year. An emergency department with beds and staff to treat 96 patients a day now finds itself handling as many as 120.
“We were thinking we were through the hump and thinking everything was going to be great and back to normal,” says Lee Stikeleather, the department’s manager. “And then it hit, and it hit all of a sudden.”
The volume of patients is only one challenge for Stikeleather and his staff. Another is that COVID-19 has helped fill not only his small community hospital but the larger ones in the Triangle and Greenville where it normally sends patients that need specialized care.
People who would be admitted to a room at UNC Johnston Health or transferred to a larger hospital within two or three hours are now spending two or three days in the emergency room, said Stikeleather, a registered nurse.
“Usually by three days, we can get most of them out. But it used to be a matter of hours, and now we’re talking a matter of days,” he said. “And these are people that need care, and we’re trying everything that we can to get them treated appropriately. But they need to go to the big tertiary care centers for a reason, and there’s just not that availability.”
The emergency department is the route for many patients into a hospital, and when the system is at or near capacity, this is where it backs up, said Alora Rodgers, the clinical care coordinator for the department.
“It’s not just here at Johnston, it’s everywhere — it’s Duke, it’s Rex, it’s Wake. Everywhere is just at max capacity,” Rodgers said. “What happens is that when we have to hold them in the emergency room, it bottlenecks. We have to hold these admissions here because there’s nowhere for them to go. Then it makes it more difficult to see the ER patients, because we just physically don’t have the place to see them.”
UNC Johnston Health is actually two community hospitals, a 50-bed hospital in Clayton and a 149-bed one in Smithfield. On Friday, the two hospitals suspended non-emergency surgeries that require an overnight stay, a move that should free up 10 beds.
It won’t be enough, said Dr. Rodney McCaskill, Johnston Health’s chief medical officer. Internal forecasts by the UNC Health system show the number of COVID-19 patients needing hospitalization will continue to grow into early October.
Hospitals say a wide majority of COVID-19 patients who end up in the hospital have not been vaccinated. In Johnston County, only 40% of residents are fully vaccinated against COVID-19, less than the statewide average of 48% and considerably less than the 60% rate in neighboring Wake County.
“Today, we have 60 patients with COVID-19, and we anticipate these numbers will continue to climb as the more contagious delta variant spreads among the unvaccinated in our communities,” McCaskill said. “Most of our patients hospitalized with COVID-19 are unvaccinated.”
Subtracting units for mental health and obstetrics, Johnston Health has beds for 149 acute care patients. As of Friday, 40% of those beds were occupied by COVID-19 patients, said Tom Williams, the president and CEO.
Like other hospitals in North Carolina, Johnston Health has been here before. Statewide, COVID-19 hospitalizations in the state peaked in mid-January, at just below 4,000. On Friday, 3,147 people with COVID-19 were hospitalized, according to the state Department of Health and Human Services.
But the resurgence of COVID-19 this summer was much more sudden than the first wave. A month ago, Johnston Health had just four COVID patients, Williams said.
“At our peak last year, which happened around Christmas, we got up to about 72 patients, but it took nine months to get there,” he said. “And we’ve hit 60 in four weeks. So that’s the scary part and why we all feel a little bit overwhelmed is how rapidly it has come upon us.”
Wait times are ‘too long’
The emergency department at the Clayton hospital performs the usual triage of patients, taking the most serious ones first and letting those who can wait sit in the lobby. Stikeleather says he goes out every couple of hours to explain the situation and encourage those who are there for something routine, such as coronavirus test, to go elsewhere.
Some people leave after waiting a long time, which worries him.
“Our wait times, I try to keep that below two hours,” he said. “Here lately it’s been five hours, six hours, sometimes longer, which is too long.”
This wave of COVID-19 patients differs from the first in several ways, Stikeleather said. For starters, there are more kids; he recalls a 16-year-old who needed to be put on a mechanical ventilator, and another teen with COVID-19 whose lung had collapsed.
The more contagious strain of the delta virus also means they’re treating entire families at once, rather than one or two members. And there are more people coming in with mental health issues, most often depression.
Stikeleather said the department could see more patients with more staff. But as the COVID-19 pandemic stretches deep into its second year, turnover of nurses and other health care workers has become a national crisis. The UNC Health Care system alone, which includes a dozen hospitals across the state, has openings for about 1,100 registered nurses.
“I send out pleas every day and get very few responses, even offering lots of money,” Stikeleather said. “People are money hungry, and when the money’s not getting them in here, that’s an issue. That’s another sign that people are stressed.”
The ICU is full of COVID patients
Up on the hospital’s second floor, the 10-bed intensive care unit, which normally treats people with all kinds of ailments that need special attention, is completely full of COVID-19 patients.
The ICU manager, registered nurse Casey Nunnery, moves patients in and out of the ICU as needed, sending someone whose condition has improved up to the COVID unit on the third floor in exchange for someone who needs more attention.
“We’re at a very scary point now. We have these patients who are very critically ill that need to be here. But there’s only so many beds,” Nunnery said. “We have to shuffle them to make sure they’re getting the appropriate level of care.”
Like the emergency department, the ICU would normally send patients who need specialized care to larger hospitals, but that’s become difficult.
“Recently, we’ve tried UNC. We’ve tried Duke. We’ve tried WakeMed. Rex. We’ve had to try all different places, but there is nowhere,” Nunnery said. “They’re taking care of their own patients. They’ve got their own backups in their EDs.”
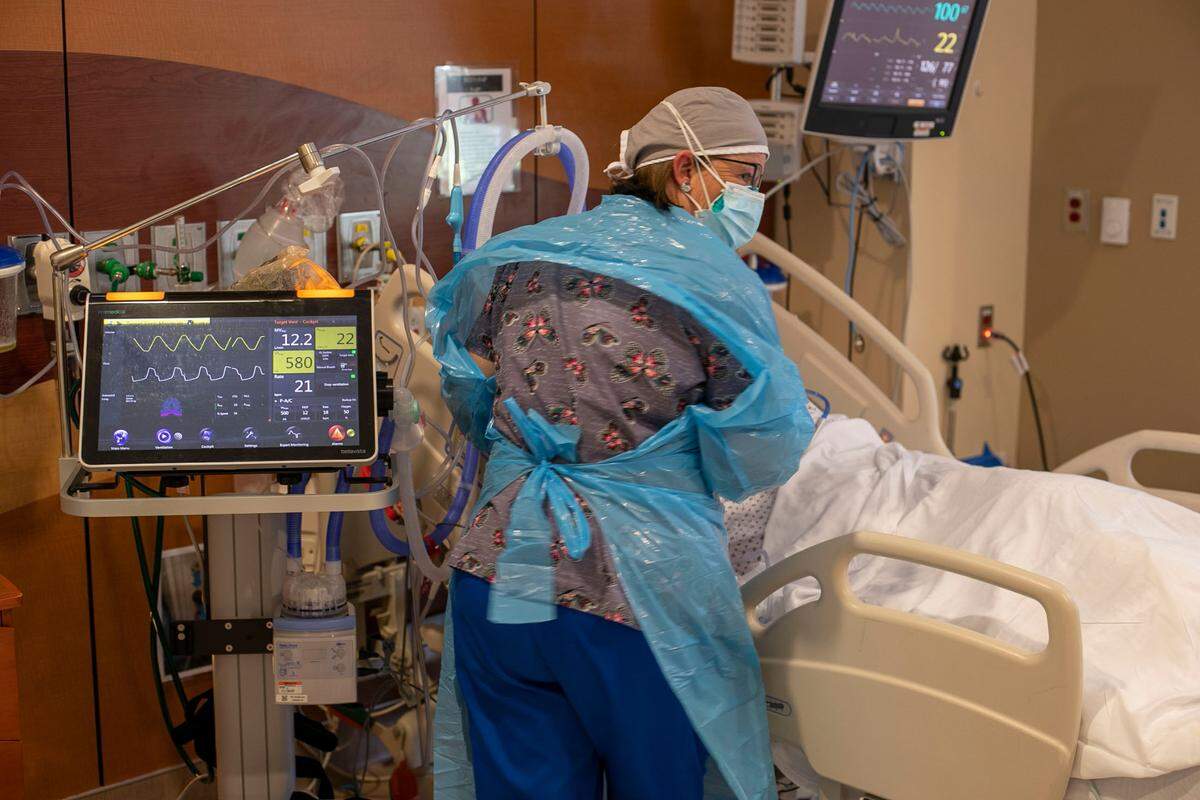
COVID-19 is a respiratory illness that makes it difficult to breathe and absorb enough oxygen in the lungs. Many hospitalized patients receive supplemental oxygen, while the sickest need mechanical ventilators to breathe for them. Statewide, more than 14,000 have died of the disease, including 233 in the last week.
COVID-19 patients tend to remain in the hospital longer, which makes the backups in the emergency rooms and ICUs slower to clear. Williams, the Johnston Health president, worries about the ripple effects.
“I think about all the people who don’t have COVID, that had strokes and heart conditions and COPD and diabetic episodes, and they’re not going to get timely care,” he said. “And what do we do? And the answer is, you do the best you can, because WakeMed and Rex and UNC and Vidant, everybody’s looking at the same numbers. They’re having the same things happen.”
All of this takes a toll on nurses, therapists and other hospital workers. Stikeleather gets emotional as he talks about members of his staff crying before their shift starts because of the stress they’re under.
The ICU converted a mail room into a staff refuge, a place to take five minutes of quiet time, an idea that came up during a meeting with the chaplain after the last wave of COVID. There’s soothing music, a selection of teas and chocolate, Play-Doh and soap bubbles and rocks on which staff members can write their concerns or a patient’s name and then place in a basin of water, where the ink washes off.
Nunnery says they call it a respite room. It will likely get used often in the weeks ahead.
“I had a nurse in tears when she saw it for the first time yesterday,” Nunnery said. “It just means a lot.”
This story was originally published August 23, 2021 at 5:45 AM.
