NC wanted to share information on drug pricing. Here’s how it got shot down.
For a brief few weeks, N.C. State Health Plan members had a rare window into the secretive world of drug pricing.
Days before the health plan trustees met to discuss whether the plan could afford to continue covering obesity medications manufactured by pharmaceutical giant Novo Nordisk, staff posted online pages of pricing information they had prepared based on an analysis of expenditures.
Notably, the documents estimated the discount, or “rebate,” Novo Nordisk had agreed to give NCSHP for these drugs — a piece of information that is largely considered a trade secret in the pharmaceutical industry.
But in a letter sent to the plan’s Board of Trustees, Sam Watts, the director of the plan, said the original documents had been taken off line and replaced with new documents, in which the “actual cost” of the drugs had been masked. Watts said the change was made under pressure from the health plan’s pharmacy benefit manager, CVS Caremark, which acts as a middleman between the plan and drug manufacturers.
Also, a revised recording of last month’s State Health Plan meeting was uploaded with discussions related to the prices in the documents cut out.
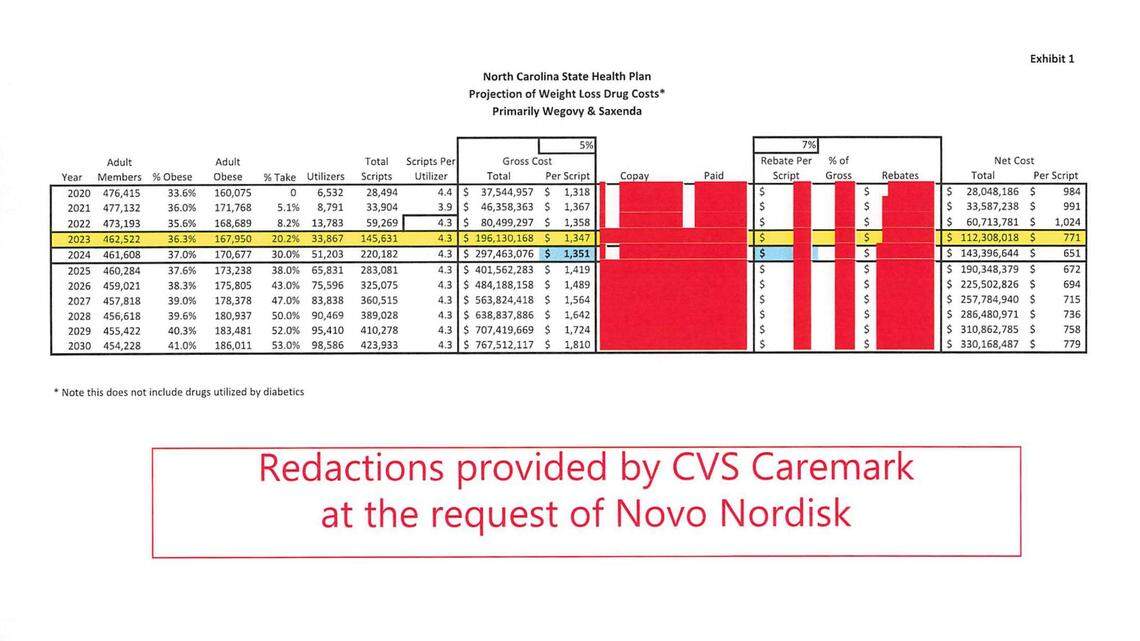
The documents from the meeting were re-uploaded with red boxes covering lines of dollar amounts. At the top of the page, the redactions have a disclaimer: “at the request of Novo Nordisk.”
“We feel this approach provides a bit of sunshine on the source of the opposition to our transparency,” Watts wrote in the letter.
Nicole Ferreira, a spokesperson for Novo Nordisk, said she was unaware of the company making any threat of legal action regarding the publication of these numbers.
A spokesperson from CVS Caremark said the company provided the health plan with “the information they need to maintain an affordable pharmacy benefit.”
State Treasurer Dale Folwell, who oversees the State Health Plan, said the redactions prevent his office from transparently managing the plan.
“We have an obligation to the members and the state taxpayers to tell them how we’re spending their money,” Folwell said. “Those that teach, protect and serve — I feel like I let them down.”
What are drug rebates?
Pharmaceutical rebates work a lot like the mail-in rebate you might get after purchasing a kitchen appliance.
While prescription drugs have a “list price,” insurance companies rarely pay that full amount. Instead, drug manufacturers like Novo Nordisk agree to reimburse a certain percentage of the drug price every time a prescription is filled, offsetting the price of the medication.
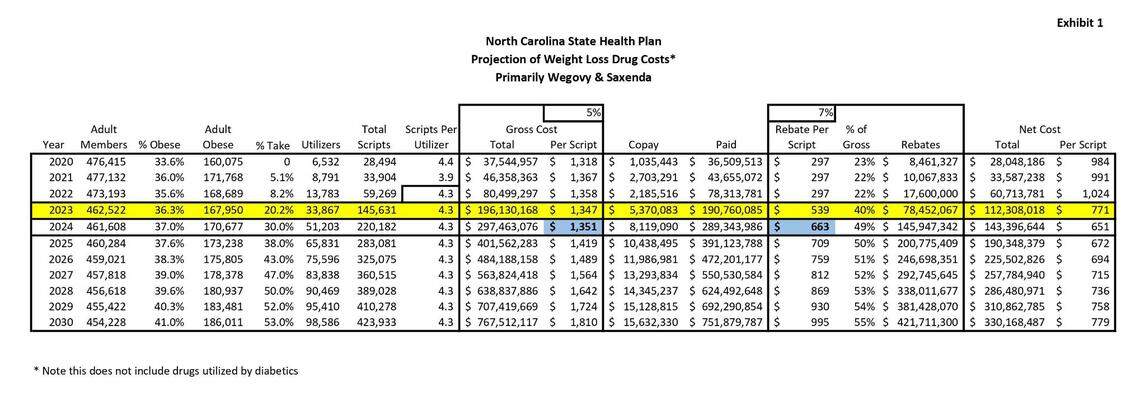
According to the State Health Plan staff analysis, Novo Nordisk gave the state a 40% rebate on Wegovy and Sexenda — two of the weight-loss drugs — in 2023. That came to a rebate of $539 on every $1,347 prescription.
Rebates allow drug manufacturers to charge different insurance plans different prices, said Matt Fielder, a health economist at the Brookings Institution.
For plans that might not otherwise include the medication on their formulary, the manufacturers can give a steep discount. Meanwhile, they can continue charging nearly full price for plans that are willing, and able, to pay more.
But that flexibility relies on each plan’s negotiated discount staying a secret, Fielder said.
“If all the rebates are public, then the plans that are getting smaller rebates will get upset and demand the same rebate,” he said.
Folwell said NCSHP staff calculated the rebate using internal spending data on the weight-loss drugs — it wasn’t information supplied by either CVS or Novo Nordisk.
Folwell said he felt it was essential to include the information to give members and trustees an accurate picture of how much these drugs cost the plan.
Fielder agreed with that assessment.
“If what they want to do is be able to weigh the full cost and benefit publicly, they’re not going to be able to do that unless they can disclose the rebates,” he said.

Some believe transparency would pressure manufacturers to give equally large rebates to all insurance plans. Other evidence suggests that publicizing rebates discourages pharmaceutical companies from giving any discounts, which would lead to plans cutting coverage of the medication.
Phillip Blando, a spokesperson for CVS Caremark, echoed that concern:
“Numerous studies show that public disclosure of drug pricing negotiations only leads to higher costs for health plans and consumers,” he wrote in statement.
Fielder said the plan’s decision to publicize the numbers might make the manufacturer hesitant to offer similar discounts to other insurance companies in the future.
But to researchers, he said, it’s still unclear whether rebate transparency would lower or raise prescription drug costs in the long run.
Teddy Rosenbluth covers science and health care for The News & Observer in a position funded by Duke Health and the Burroughs Wellcome Fund. The N&O maintains full editorial control of the work.
