NC could see a measles outbreak soon. We talked to infectious disease experts
AI-generated summary reviewed by our newsroom.
- North Carolina reports no confirmed measles cases; experts warn arrivals likely.
- MMR vaccination prevents measles; unvaccinated people account for most U.S. cases.
- Use North Carolina immunization registry and seek postexposure MMR within 72 hours.
South Carolina is experiencing a measles outbreak, and we’re wondering if North Carolina will start to see that here soon too.
The News & Observer spoke with Dr. David Weber (Medical Director of UNC Medical Center’s Department of Infection Prevention) and Dr. David Wohl (Professor of Medicine in UNC’s Division of Infectious Diseases) to learn more about the current measles outbreak and North Carolina’s risk.
Is measles in NC?
North Carolina does not currently have any confirmed measles cases, according to the NC Department of Health & Human Services’ website (as of Friday, Dec. 12 afternoon).
A measles case was confirmed this summer. Before that, a case was confirmed fall 2024, but there were no reported cases from 2019 to 2023, per NCDHHS.

Could NC see a measles outbreak?
It’s very likely North Carolina will begin to see measles cases over the next few weeks, Weber said.
Holiday travel can bring diseases from other parts of the country (like South Carolina) to our state, and the winter weather is driving gatherings indoors without much ventilation.
“[Measles] will most likely show up here eventually. It is a matter of time,” Wohl said.
South Carolina’s Department of Public Health has reported 129 cases since July. More than 125 of those are currently centered around Spartanburg County, which is roughly a 90-minute drive from Charlotte and a 4-hour drive from Raleigh.
How contagious is measles?
Extremely — measles is the most infectious disease we currently have, Weber said.
“If I’m infected and in a group of people who aren’t immunized, somewhere between 14 to 18 people would develop measles. [Illnesses] like COVID or flu would produce two to three, to put it in perspective.”
Measles have even spread through empty waiting rooms. Meaning, someone with measles was in a waiting room, then up to two hours after the infected person left the waiting room, someone else entered and got measles from the particles hanging around the air, Weber said. This doesn’t occur with other respiratory illnesses, like flu or COVID.
How to treat measles?
There’s no antiviral treatment for measles, according to the Mayo Clinic. It’s advised to rest, drink plenty of fluids and eat nutritious foods.
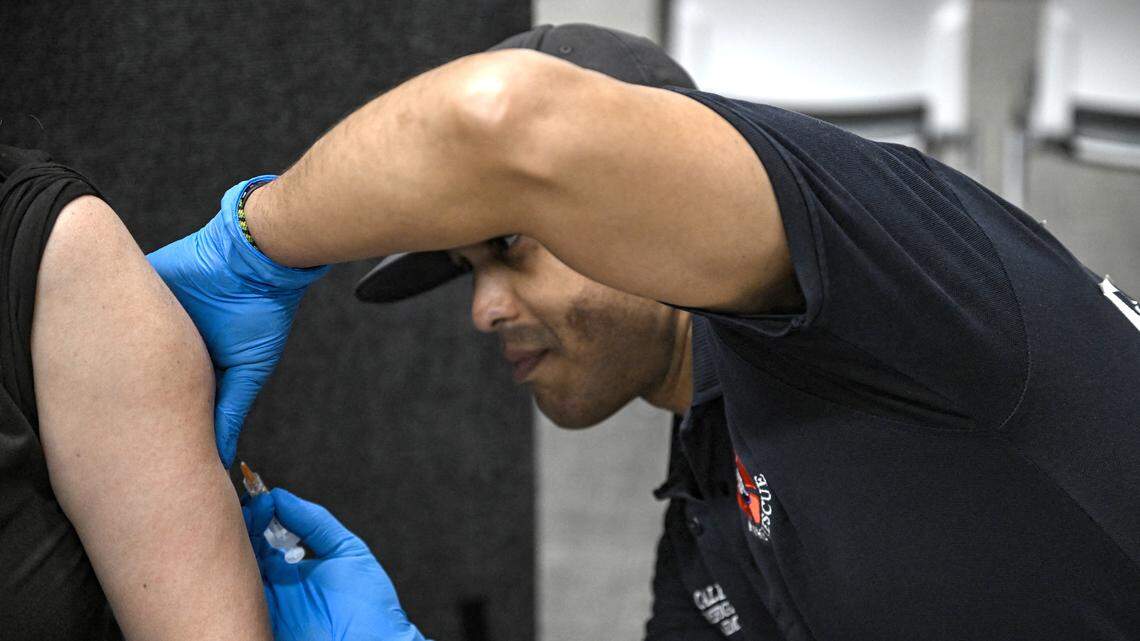
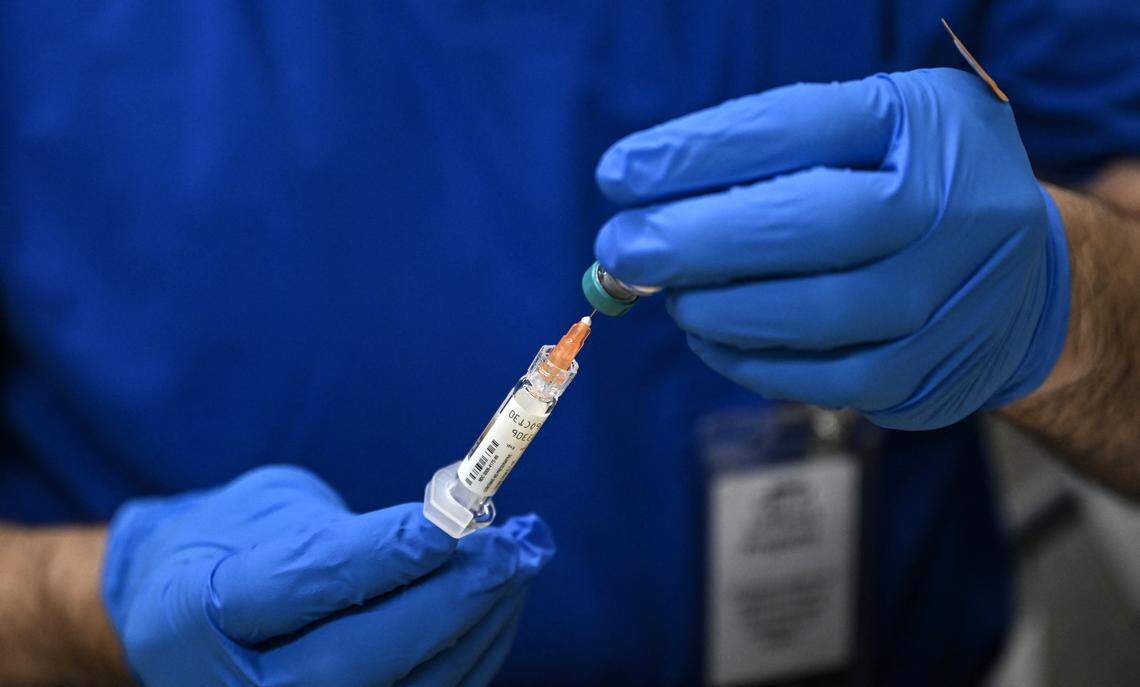
(Almost) anyone exposed to measles can get vaccinated within 72 hours of the exposure, which will “reduce your risk tremendously,” Weber said. Those who can’t get the vaccine are able to get immune globulin (essentially an antibody booster) to reduce the risk of infection too.
“Many with severe measles develop infection of the lungs, which requires oxygen and sometimes ventilator support,” Wohl said.
Is measles fatal?
It can be, though it’s very rare.
According to data from the Centers for Disease Control and Prevention (as of Wednesday, Dec. 10):
- More than 1,900 measles cases were reported in the United States this year.
- 92% of those people were unvaccinated or did not know if they were vaccinated. 4% of those people had both MMR doses.
- 11% of cases led to hospitalization.
- 3 deaths were reported from measles.
How to prevent measles?
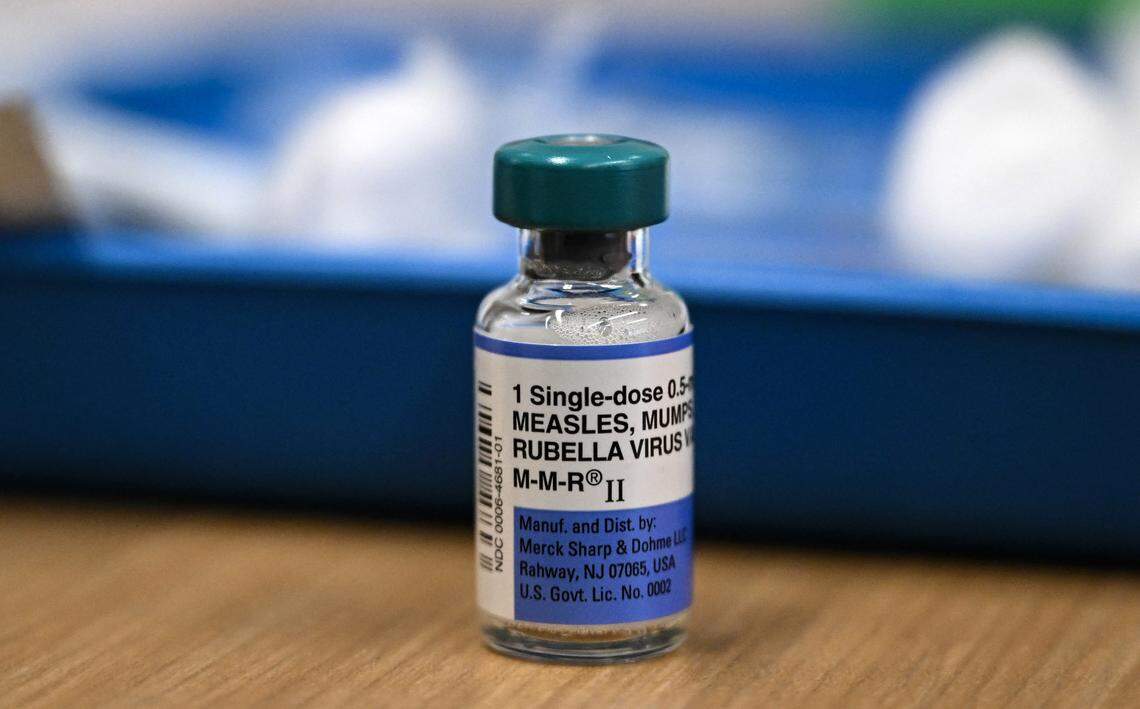
Two doses of the MMR vaccine, which protects against measles, mumps and rubella.
The vaccine is a live virus, making it recommended for most people, but not people who are immunocompromised or pregnant, Weber said.
“Measles is almost completely prevented by the MMR vaccine, which has been used for decades and is safe as well as effective,” Wohl said.
“Over 90% of the more than 1,800 measles cases in the U.S. this year have been among people who are unvaccinated or unknown to be vaccinated. One in 10 people of these U.S. measles cases has required hospitalization, and many are children.”
Do I need a measles vaccine booster?
Boosters are not recommended or required for MMR vaccines, as long as both rounds have been completed at some point in your life, Weber said.
Many received two doses (in two separate visits) as an infant, and no matter how many years it’s been since then, anyone previously immunized does not need to receive another shot, or another round of shots, Weber said.
How to know if you got your measles vaccine?
North Carolina has an Immunization Information Database, which can help people who have received vaccinations in the state locate their records.
The NC Division of Public Health recommends people searching for their immunization records:
- Contact their vaccination provider who can use the immunization registry to learn when and which vaccines you’ve received in North Carolina.
- Check school or military records, as most K-12 schools and colleges keep immunization records on file. (These may be on file for one or two years after graduation or transferring.)
- Check family records, including baby books, camp applications or other old medical records.
Visit dph.ncdhhs.gov/programs/epidemiology/immunization to learn more about how this works.
While not every state has the same database, you can search where to get more information about finding each state’s vaccination records at cdc.gov/iis.
If you still can’t find your records, you’re considered susceptible to disease, the Division of Public Health says. It’s recommended you get vaccinated again, noting it’s not harmful to get additional vaccines.
How to know if you have measles?
It can be difficult to discern measles from other wintertime viruses, like the flu or COVID. But measles often comes with a telltale rash.
Three to five days after the standard winter sickness symptoms (cough, red eyes, runny nose) kick in, it’s common to get a rash. These are usually small, raised bumps that appear on top of flat, red spots. They often spread first from the head/face to the rest of the body. High fevers are also common, Weber said.
Other diseases, like chicken pox, also have similar symptoms. If you experience all these symptoms, it’s best to contact your healthcare provider for an evaluation, diagnosis and treatment plan, Weber said.
This story was originally published December 12, 2025 at 1:34 PM.