12 hours in a 24/7 crisis: How a NC ER nurse feels COVID’s looming presence even in its absence
READ MORE
12 hours in a 24/7 crisis
What has COVID’s looming presence done to nurses in North Carolina? While coronavirus cases stay in flux and staffing shortages remain in hospitals, nurses are working on how to navigate. This is The News & Observer’s special report.
Expand All
12 hours in a 24/7 crisis: How a NC ER nurse feels COVID’s looming presence even in its absence
NC Nursing students learn to care for others, themselves as worker shortage, COVID continue

When should you visit the ER vs. urgent care? Raleigh expert weighs in
‘Choice of jobs’: As COVID takes a toll on nurses, some turn to lucrative travel jobs
Imagining the features of her co-workers’ faces, which she had never seen unmasked, Erica Jones South always got the noses wrong.
South, a registered nurse, started work at UNC Rex Healthcare’s emergency department in September 2020, six months into the pandemic. By then, face coverings had become part of the uniform.
Masks slowed the spread of infection, but they created a sense of estrangement, putting a distance between employees and patients much greater than the thickness of the material.
To compensate, a hospital volunteer group invited Rex employees to submit bare-faced photos of themselves and put those on buttons the workers could pin to their scrubs. It was the first time South and many others got to see the contours that make their colleagues’ faces unique.
“Cheekbones,” South said. “And some of the men had facial hair. I had no idea. It was amazing.”
The buttons eventually fell apart. Meanwhile, the pandemic wears on.
It surged in August and September on a wave of the delta variant, peaking in North Carolina on Sept. 11 with a one-day count of 11,337 new cases. Then it subsided, as it may be doing now, dropping to 2,219 new daily cases on Oct. 4, giving health care workers a breather and a sense of hope.
But even on a rare day like the first Friday in October, when no one presented at the Rex ER during South’s shift with just complaints of symptoms from COVID-19, the threat of the virus lurked in the background, like the smell of rubbing alcohol and the pinging of heart monitors.
That night, the nation passed the milestone of 700,000 COVID-19-related deaths.
The specter of infection looms and shapes nearly every aspect of life in the emergency department, where the crew still is learning how to keep people from dying with COVID at the same time they’re learning to live with it.
Here comes the bride
Every time they clock in, emergency department staff know this could be the shift when they get COVID-19.
South — whose last name still would be Jones for eight more days — was especially aware of the risk as she arrived for the start of her shift last Friday, trailed for the day by a News & Observer photographer and reporter. So were her co-workers, some of whom were surprised to see her.
“Aren’t you about to get married?” one asked when she came onto the floor.
“Yes!” South said, her face turning pink with excitement above her surgical mask. “Next Saturday. I can’t wait!”
Then she set down her tall glass of iced coffee, turned to the nurse whose shift was ending, whose patients would now become South’s patients, and said, “Tell me all the things.”
A year ago, couples were canceling weddings because of COVID-19. Family reunions and vacations went by the wayside along with concerts and theater performances and regular hours for nearly every kind of business in America.
People even quit going to emergency rooms and their own doctors’ offices, putting off treatment they should have had.
Now there’s the delta variant surge. Coming after a few halcyon weeks of reduced spread in early summer, it’s been hard on health care workers, and not just because it filled emergency departments back to overflowing.
“We had that peak last winter and hoped to see things die down when the vaccines came out,” South said. “We had such high hopes with the lower numbers in the summer, especially at the emergency department. But then the new variant hit.
“I think we had hoped that more people would get vaccinated.”
As case numbers and deaths soared with the delta variant, “We thought about canceling the wedding,” South said of her and her fiance. “With COVID peaking, we weren’t sure how it was going to work with people traveling.”
Both South and her fiance had been vaccinated. The wedding and reception would be outside, near Stone Mountain, with only 20 guests. South encouraged them all to get vaccinated and, as the venue suggested, required everyone to have a negative COVID test within 72 hours of the event. Food and utensils were individually wrapped to avoid cross-contamination in case someone unknowingly carried the virus.
“We decided to go ahead,” South said with a life-must-go-on tone. “We’re pretty comfortable that it’s going to be the safest event possible.”
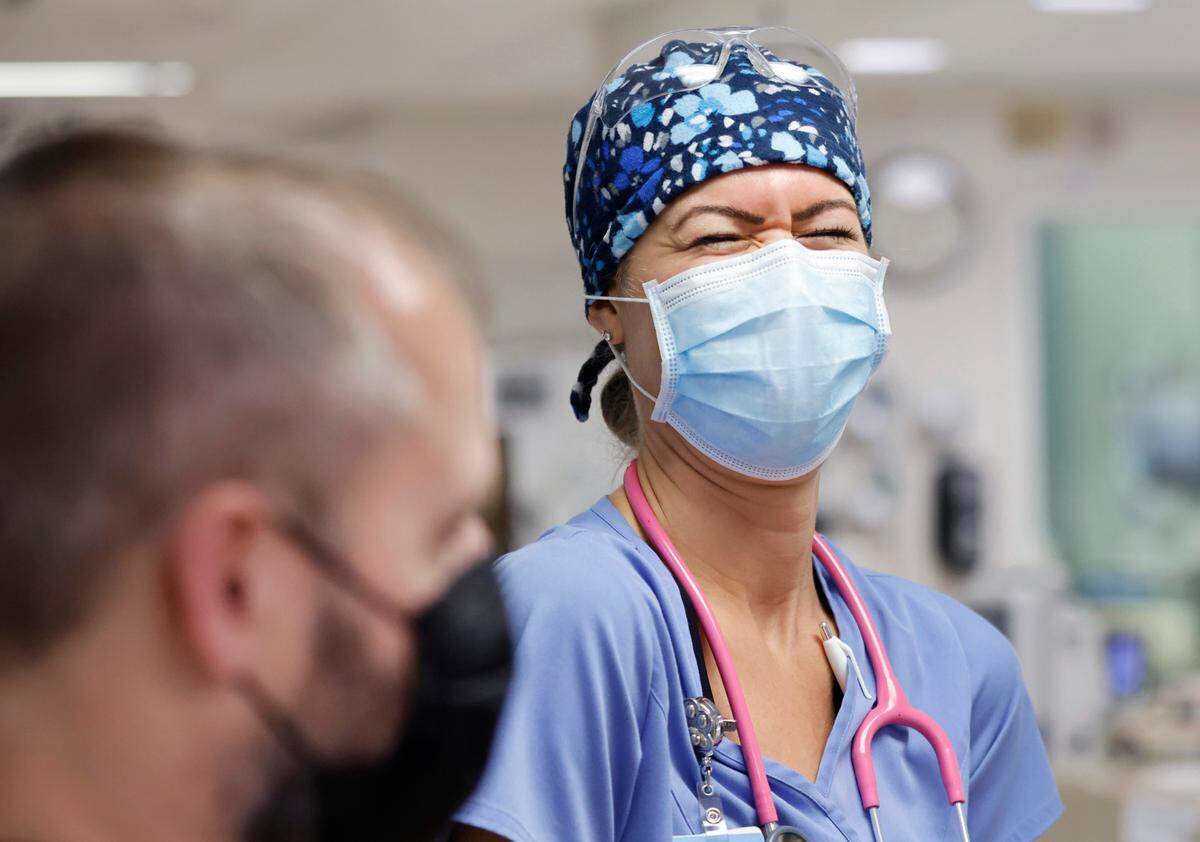
Taking for granted the human touch
Like many nurses, South works three 12-hour shifts per week, always Friday, Saturday and Sunday, 11 a.m. to 11 p.m., unless she takes extra hours to help out when needed.
“I like this shift because it tends to be pretty busy,” South said, pulling on gloves and rubbing a sanitizing wipe across her computer keyboard, her phone and her section of the long counter at the nurses’ station. Just another precaution.
South, 27, rarely sits during her shift, perching only long enough to scan her computer, looking for orders that need to be put in or to document patient information. Even then, with her free hand, she fidgets with her hospital badges or tweaks the rubber straps on the respirator mask in her pocket.
Heavier and hotter than a surgical mask, the respirator one offers better protection if a COVID patient comes in. She can simultaneously strap on the respirator while peeling off the surgical mask without ever exposing her face, kind of the way Jennifer Beals shimmied out of her bra in “Flashdance” in 1983.
Armed with updates on what’s happening with her patients, South goes immediately to introduce herself to each one, ask them a few questions and answer any they might have.
Early in this shift, she had a patient with severe stomach pain, one with trouble in her back and one with unexplained tingling in the limbs.
“Patients are often very anxious, which makes them feel even worse,” South said. “What I try to do is find out first why they’re anxious: Have they had too much medication? Have they not had enough medication? Is it a child who’s missing Mom? Is there a hormonal problem?
“There is usually something out of balance, and I try to figure out what it is.”
Sometimes, South said, “They just need somebody to talk to, and the best thing you can do is sit and listen.”
Raised in Chicago and schooled in Wisconsin, South has an easy Midwestern charm. Where Southern nurses might call their patients “honey,” “darlin’” or “sweetheart,” she addresses all of hers as “my dear.”
Because of COVID, she said, nurses have had to learn new ways of comforting patients, calming them, building trust.
“One thing that has really changed in the health care world that maybe we took for granted before is just human touch itself,” she said. “That is such a healing process when you have a patient who doesn’t feel well or they’ve gotten some bad news. Just holding their hand. Sometimes words just don’t provide that comfort.
“It’s just being next to them, letting them know ‘I’m here for you. I can’t fix this right now and this is going to be a long process.’
“We’ve all gotten better at showing emotion just through our eyes,” South said, “but sometimes just being able to hold their hand is really important. And holding a glove is different than holding a hand.
“With these COVID patients, we just can’t risk that exposure.”
EMS on the way: Stroke alert
On average, Rex’s emergency department gets 10 to 12 patients per hour in the mornings. Evenings sometimes are busier before traffic drops off in the middle of the night, said Danny Yoder, emergency department nurse manager.
In response to COVID, Rex expanded the emergency department into other areas of the floor, including some that used to be hallways, and added a climate-controlled tent in the parking lot near the big red “Emergency” sign.
Right now, the tent gives family members a place out of the weather to wait while patients get processed, but it could be used for patients, along with a total of 48 rooms now designated for the emergency department.
To reduce the spread of COVID, the hospital built new treatment rooms with doors instead of curtains, and it can set the pressure inside them lower than the pressure outside so contaminated air doesn’t seep out when the door opens..
On this shift, South had primary responsibility for patients in four curtained stalls of the emergency department and was on standby to help treat any “code” patients arriving by ambulance under suspicion of a heart attack, stroke or other life-threatening event.
The first code of South’s day came shortly after noon, starting as a radio call from Wake County Emergency Medical Services directly to the charge nurse and then as a general alert heard throughout the hospital to summon code team members.
South swooped into action, heading for the landing area just inside the two front doors. Other team members began arriving and getting ready: doctor, pharmacist, respiratory therapist.
Then, before the first code case could get there, a second, identical call came in, meaning that now two patients — two possible strokes — would land at the same time.
The first team instantly split into two teams, and in minutes, both patients had arrived, had been stabilized and had been sent for imaging. It was a swarm of maybe a dozen people, all arms and blue-gloved hands and syringes and tubes and no idea whether either patient was carrying a virus that could make anyone working to save them gravely ill.

Detectives at work
For South, it feels natural to borrow language from police work for use in health care. An affliction becomes a case, and the effort to identify the problem is an investigation.
“We’re like detectives,” South said. “We’re gathering clues, getting all the information we can: What could go wrong that would cause this? You want to start with, ‘What is the worst-case scenario?’ because you want to prevent the worst-case scenario. You start with that and work down the list of other possible causes.
“It’s like trying to solve a mystery.”
While she was working on the code patient, a colleague automatically took over South’s other patients. It’s part of the team approach Rex uses and a main reason South chose the hospital when she decided to stop working as a travel nurse.
“We have so many resources here,” she said, speaking more of the hospital’s people than its equipment. With a statewide nursing shortage made worse by the pandemic, South said Rex leans on fluidity, moving people around quickly to respond to the most pressing needs.
Some nurses have felt overwhelmed during the pandemic, and workforce experts say they expect many to retire early or change careers because of what they call “moral distress.” That’s when conditions prevent them from giving the kind of care they are trained to provide.
Because of Rex’s approach, South said, when the two suspected stroke patients were wheeled to the next stop, ”I have the peace of mind that we gave them the very best care we could.”
Once they were gone, South resumed care for her patients. Throughout the afternoon, a few were admitted and moved upstairs into regular rooms, where other staff would take over the investigative work that started here. Others were treated in the emergency department and went home.
Because the COVID-19 virus is such a changeling, hospital policies and practices are constantly in flux as well, sometimes hour by hour. At the moment, Rex was requiring COVID tests only of patients being admitted to the hospital. Patients discharged from there were tested for COVID only if they had symptoms.
During this day’s shift, that meant dozens of patients came and went through the emergency department who might have been carrying the virus.
COVID on their minds
Around 5 p.m., South took her 30-minute meal break. She doesn’t eat breakfast and said, “When I’m busy, I’m not hungry,” so this was her first meal of the day. It was the one she brings most days: a bowl of shredded lettuce with broccoli and carrots, and a fresh apple.
She went into the break room and reflexively turned off the wall-mounted TV. She hates the noise.
The room was filled with clutter. Old coats on a rack. A box of donated cookies and snacks. Thank-you notes taped to the wall. There was a couch with a blanket and pillows.
If this place away from the public eye used to be where nurses bonded, it’s not anymore. Because of COVID, only two or three people are allowed to take a break at the same time to avoid overcrowding in the break room.
Now, South said, staff members bond on the emergency department floor, sometimes over the shared experience of white-knuckled, all-hands-on-deck responses to medical emergencies most never dreamed they would see in their careers.
Near the end of this relatively slow day, while South was trying to expedite a patient’s blood transfusion held up by a computer glitch, she got a chance to flex her medical muscle. The alert came in for a patient who had been discovered unresponsive at home by friends. The last time the patient had been “known well” was at least 24 hours before.
“This is what I live for,” South said, rushing to the front door to get ready to meet the code team.
As soon as the patient landed, the blue-gloved hands went to work. South called immediately to move the patient into the code room, where the team would have all its tools at hand.
It looked bleak. The patient, in their mid-50s, had lain unconscious for so long that the skin had begun to break down. Blood pressure was dangerously high. South put in a line for intravenous medications and started drugs to work on that and to sedate the patient enough to tolerate a breathing tube. Then she and two others on the team headed off for a CT scan, where another team took over and quickly found a brain bleed. After a short time back in the emergency department, the patient was taken to intensive care.
South went straight to work cleaning up the code room, picking up wrappers from medical gear and putting equipment back in order. As soon as she finished, another ambulance team brought in a second unresponsive patient, this one in their 80s, and the team went through the same process again.
Soon after she went into nursing, South said, she realized the only way she could live with the gravity of the work would be to believe in the most hopeful outcome for every patient. That’s easier to do in the emergency department than in some other parts of the hospital because once a patient leaves that department, South generally doesn’t know how their case progresses. Patient privacy rules don’t allow her to go checking on them a day or two later.
“For my own sake, I like to think the best,” she said, including about the work she and her team did to help.
‘The threat of COVID’
South is training as a triage nurse to expand her usefulness in the hospital, and she plans eventually to learn both Spanish and American Sign Language in service of patients. She said she always wants to continue to improve her nursing skills, so she reviews cases in her mind to make sure she did everything she was trained to do.
“But you can’t beat yourself up with what-ifs,” she said. “It’s something you have to come to terms with. You made the best decisions you could with the information you had.”
It’s been the same working through the pandemic, she said.
“The threat of COVID, I think it’s always in the back of our minds. We have those symptomatic patients, and it’s obvious. And then we have the ones who don’t have symptoms, and we wonder, ‘Do they have it and they’re just not showing symptoms yet?’
“We don’t want to get sick, and we don’t want to take COVID home to our families,” South said. But when she’s focused on the mystery, thinking what to do next to help the patient in front of her, “I guess I just put it out of my mind.”
This story was originally published October 10, 2021 at 6:00 AM with the headline "12 hours in a 24/7 crisis: How a NC ER nurse feels COVID’s looming presence even in its absence."