Overhaul of NC’s health plan could cut costs, depending on which provider you pick
AI-generated summary reviewed by our newsroom.
- The State Health Plan approved a three‑tier network structure.
- Preferred providers get more patients while members pay less. Non‑preferred costs more.
- The board approved the structure; cost details due in June.
Many North Carolina state employees could soon receive more of their health care through a structure that encourages them to choose certain providers to achieve savings for both themselves and the plan.
That follows a vote Tuesday by the State Health Plan Board of Trustees approving the implementation of a three-tier network structure.
“The fundamental principle we’re talking about is steering patient volume to those who want to work with the State Health Plan for access and pricing,” said Thomas Friedman, the plan’s executive administrator. “We cannot let providers charge whatever they want for things and get the same access to patients.”
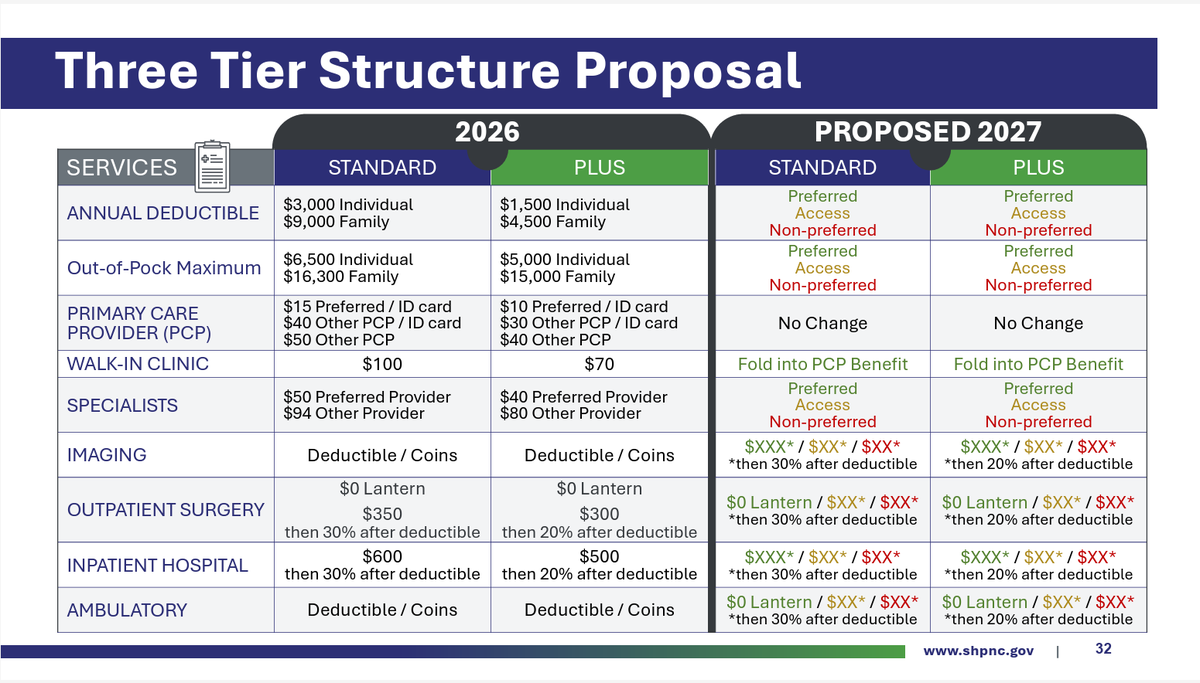
The three tiers will be:
- Preferred
- Access
- Non-preferred
Members and the plan would pay less when preferred providers are used, and more when non-preferred providers are used. Preferred providers, meanwhile, would get more patients.
The State Health Plan provides health insurance for more than 750,000 state workers, retirees and their family members.
Earlier this year, the plan’s board of trustees had already approved contracts with three clinically integrated networks, or groups of health care providers: Aledade, Community Care Physician Network and UNC Health Alliance. When members go to these providers, they see savings.
The plan also launched last year a surgical benefit with Lantern, a specialty care platform, to offer certain surgeries at no cost to members. The plan pays less when these providers are used. Novant Health and EmergeOrtho joined that partnership.
The next phase of that expansion will include maternity care, dermatology and independent pharmacy services, according to plan documents.
The vote was not on specific cost-sharing amounts, but rather to approve the structure. No final decision on costs will come until June. But the vote allows operational work to begin and also strengthens the plan’s position in negotiations, Friedman said.
Friedman noted that access to care is not equitable across the state, with most care concentrated in about 10 of North Carolina’s 100 counties. Many people are traveling to receive care. For example, among State Health Plan members last year, about 70% received care in 10 counties. That includes Wake County.
“If you have 24 options for imaging in Wake County from different locations, we can make it very cheap to go to three, and we want to make it three and keep the middle kind of what it is — but we need to get better prices and use our scale to get those better prices,” he said.
He said that the “access tier” would preserve benefits.
If providers in the preferred tier are not able to meet all needs, “then we can’t punish everyone else,” Friedman said. “We have to maintain that current access tier where it’s like, ‘Hey, your benefit is not changing that much from year to year.’”
The plan will have the ability to “badge” providers so that members can see who is a preferred provider and who is not, which can be especially helpful at the time of open enrollment when members are choosing their plan, State Health Plan staff said.
Premiums
Another idea proposed during the meeting was tying premium increases for active employees to the percentage raises that employees receive.
Friedman said that was a “long-term strategy. This is what we are building toward.”
Any votes on premiums for future years would happen in July, said Friedman.
Last August, the board voted for the first time in years to increase premiums for 2026. The premium increases were tied to salaries, with the lowest rates for employees earning under $50,000 and the highest rates for those making more than $90,000.
Friedman said that a member of the State Health Plan who makes $55,000 a year and chooses individual coverage is currently paying either $94 a month on the Plus PPO plan or $50 a month on the Standard PPO plan, which is about 1–2% of their salary.
Under a new proposal — not voted on Tuesday — if that member got a 1% raise, or $550, then the Plus premium would go up by 1% to $94.94 and $50.50.
“I know it would feel better if it were a fixed dollar amount, but we can’t,” State Treasurer Brad Briner said. “When you have a 6% medical trend (the projected increase in health care costs from one year to the next) and other things, over time, it breaks, and that’s where we were two years ago.”
“But we can make the commitment to keep these as a percentage of salary consistent. Nobody else is making that commitment,” said Briner, who is a Republican and took office last January.
The premium increases already enacted and any future ones, as well as the latest changes, follow the plan’s closing of a $500 million deficit that had been projected for 2026.
The plan’s also tackling a $1.4 billion deficit projected for 2027.
Opening bids
The State Health Plan is also poised to issue a new request for proposals — or an invitation for vendors to submit bids to take over administration of the State Health Plan in 2028. That contract is currently held by Aetna.
The State Health Plan also issued a request for proposals last month for the plan’s pharmacy benefit manager contract, currently held by CVS Caremark.
Asked by The News & Observer about the decision not to extend the Aetna contract, Friedman said on Monday that “the administration has different priorities from the previous administration, and the contract is up after three years, so that is what we’re focused on right now.”
Friedman said Tuesday that it is in active negotiations with the state’s independent pharmacy association, which has built a network across the state.
Friedman said that the plan is requiring bidders that want to be the plan’s pharmacy benefit manager — which processes pharmacy claims that the state then reimburses — to give the plan flexibility to treat independent pharmacies differently than major pharmacies.
“That is a requirement that we are putting on whomever is going to be our next pharmacy benefit manager, to allow us that control and flexibility,” Friedman said.
SHP spokesperson Loretta Boniti previously told The N&O the plan was in a “silent period” for the PBM contract, restricting staff from discussing the procurement.
Phillip Blando, a spokesperson for Aetna and CVS Caremark parent company CVS Health previously told The N&O that the company works to “improve health outcomes for members while containing costs in one of the most expensive health care markets in the country.”
Friedman said the SHP contract should be awarded in July and the PBM contract in June or July.
