In Triangle hospitals, relief at COVID’s decline but also concern it may not last
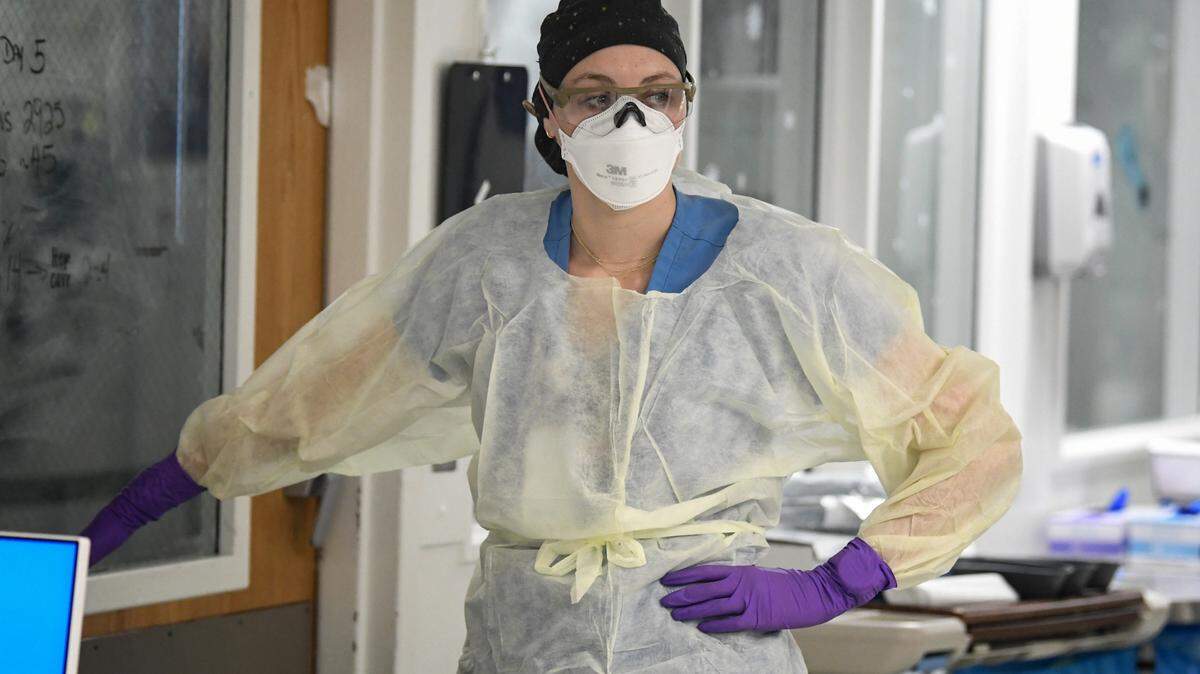
A dramatic drop in new COVID-19 cases has prompted state and local governments and school boards to stop requiring people to wear masks. Throw in the return of spring weather, and people are as optimistic as ever that the coronavirus pandemic may be over.
There’s some of that same optimism in Triangle hospitals, where the number of patients admitted with COVID-19 has dropped dramatically in the last month. But that feeling is tempered by the knowledge that we’ve been here before, with a disease that seemed in retreat only to come roaring back again.
The number of people hospitalized with COVID-19 in North Carolina has dropped from more than 5,100 in late January to 1,336 on Friday, according to the state Department of Health and Human Services. At hospitals across the state, there’s a sense of relief among workers who have endured one crisis after another over the past two years.
People are smiling again and having the kind of routine meetings and celebrations that just didn’t happen when the hospital was besieged with COVID-19 patients, said Dr. David Kirk, a pulmonologist and critical care specialist at WakeMed. The number of COVID-19 patients at WakeMed has dropped from 220 in January to 42 on Wednesday.
That same day, Kirk said he met with people who run WakeMed’s intensive care units to talk about how to make them better.
“These are the kind of decisions and discussions that require people to sit down and have a cup of coffee and think,” he said. “And man, for the last little while we’ve not had even that little bit of bandwidth to actually do those types of things.”
Morale is improving at UNC Johnston hospitals in Smithfield and Clayton, where at one point this winter two-thirds of medical inpatient beds were occupied by COVID-19 patients, said Dr. Rodney McCaskill, the medical director. COVID-19 cases have dropped from 90 to 15, and the emergency department that was overwhelmed with coronavirus patients in December is back to normal, McCaskill said.
But no one in the hospitals is certain the pandemic is over, he said.
“We felt like this might be over eight months ago, right? Or six months ago, and we had the highest peak we’ve ever had immediately following,” he said. “So I think to feel like it’s over is premature. It might be, but that’s what we thought six months ago.”
The Triangle’s large medical centers have COVID-19 patients enduring long recoveries from severe bouts with the disease. Duke University Hospital in Durham has COVID patients who have been there for months, including at least one who arrived in October, said Dr. Lisa Pickett, the chief medical officer.
UNC Medical Center in Chapel Hill has three times as many patients recovering from COVID-19 than it does new coronavirus cases coming in, said Dr. Shannon Carson, a pulmonologist and acute care specialist.
“We still have pretty significant COVID burden,” Carson said. “About half of our patients in the medical ICU still are here because of a COVID-related problem that they’re trying to recover from.”
Some patients with serious COVID-19 will not survive. In the last month, more than 1,650 people have died from the disease statewide, including 193 in the last three days. Since the pandemic began, COVID-19 has killed 22,763 people in North Carolina, according to DHHS.
We’re seeing a ‘saturation effect’
Doctors say a large majority of hospitalized COVID-19 patients are unvaccinated, and most of the few vaccinated patients had some underlying health condition that compromised their immune systems or made them more likely to get severely ill.
Since the pandemic began, people 65 and older have been most vulnerable to the disease, accounting for a majority of COVID-19 deaths in North Carolina. But they’re also the group with the highest vaccination rates, and that’s reflected in hospital patients, McCaskill said.
“If the vaccines didn’t work, they’re the ones who would all be here, vaccinated and in the ICU,” he said. “But by and large, it’s still the unvaccinated that are the ones that are in our hospital and in our ICUs.”
This winter’s spike in COVID-19 was caused by the omicron variant of the coronavirus. The prevalence of the variant has also helped drive down cases and hospitalizations, said Dr. David Wohl, an infectious disease specialist at UNC Health. That’s because the variant was very contagious but also caused less severe illness than previous ones, and it ran through the population without many people even knowing they had it, Wohl said.
“I do think what we’re seeing is a saturation effect,” he said. “Everyone who could pretty much get omicron has gotten omicron. Vaccines are protecting a lot of us from not only infection but also from severe disease. So things are looking much better.”
Kirk at WakeMed agrees.
“We’ve got a big kind of shield of immunity out there, until a new completely different variant comes through,” he said. “So we just feel that we’re gonna have a good spring and good summer.”
Hospitals are still requiring masks
The decline in hospitalizations seems to support the dropping of mask mandates, one of several measures put in place in 2020 to try to prevent COVID-19 from overwhelming the health care system.
But one place mask mandates are not going away soon is in hospitals themselves. Wohl and other doctors note that the coronavirus is still circulating in the community and that visitors could easily bring it into hospitals without knowing it.
“We really live our values of caring for our patients and our loved ones and each other by continuing to require masks,” said Pickett at Duke University Hospital. “And that’s simply because of the sick and vulnerable population of patients that we serve.”
Kirk said WakeMed is working on new signs and other measures to make sure visitors understand why they’re being required to wear masks.
“We worry that just because everybody’s not masking at Target and not masking out in restaurants that people are going to feel like they don’t really need the mask inside the hospital,” he said. “There’s going to be some people that are asymptomatic come in and visit their grandma. And if they’re not wearing a mask they may infect grandma, and that may be what tips her over the edge.”
Hospitals using this time to regroup
Hospital leaders say after two years of COVID-19, doctors, nurses and other workers are tired, both physically and emotionally. As the latest wave of cases ebbs, everyone’s getting a breather.
At the same time, hospitals need to replenish their depleted staffs. Many nurses in particular retired or quit health care during the pandemic or went to work for traveling nurse companies that paid much better.
“So this is going to be a time of nursing the soul of our team,” Pickett said, “and then rebuilding the numbers of our team.”
Carson at UNC Medical Center said the lull will allow hospitals to review how they handle COVID-19 cases and see what they might do differently next time, if there is one.
“We’re not going to let our guard down, because we’ve just learned that some new variant can pop up anywhere across the globe, and we’ve definitely seen how quickly that can spread,” Carson said. “So we’re going to be hopeful but also prepared.”
This story was originally published March 5, 2022 at 8:47 AM.
